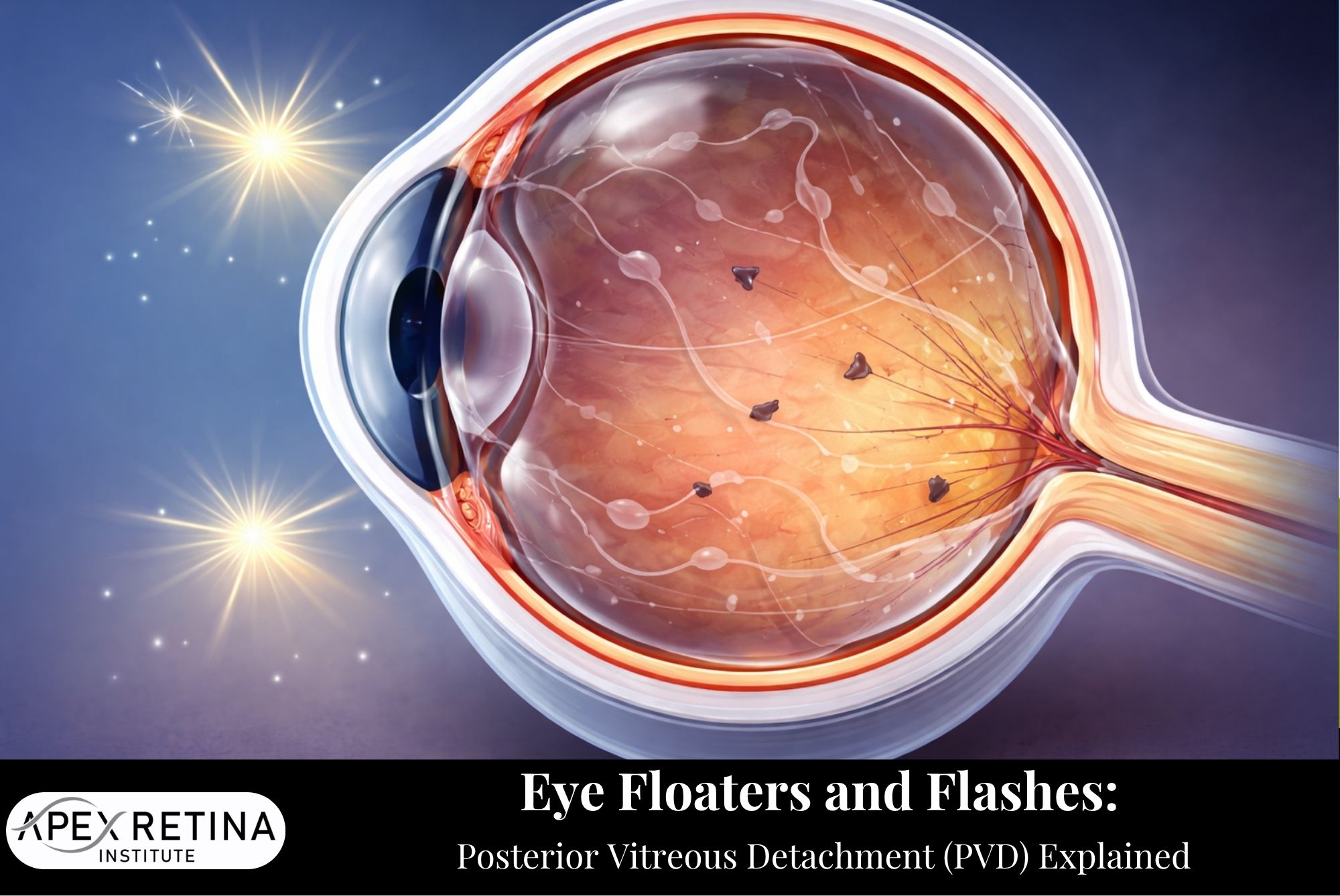
As we age, changes in our eyes are natural—but some can feel sudden and alarming. One such condition is Posterior Vitreous Detachment (PVD), a common occurrence that can cause new floaters or flashes of light in your vision. While often harmless, PVD can sometimes signal more serious eye conditions that require prompt medical attention.
At Apex Retina Institute, we specialize in diagnosing and managing retinal conditions with precision and care. In this guide, we’ll walk you through everything you need to know about PVD—what it is, what to watch for, and when to seek expert care.
What Is Posterior Vitreous Detachment?
The eye is filled with a gel-like substance called the vitreous humor, which helps maintain its shape and allows light to pass through to the retina. Over time, this gel naturally shrinks and becomes more liquid.
A Posterior Vitreous Detachment (PVD) occurs when the vitreous gel separates from the retina—the light-sensitive tissue at the back of the eye.
This is a common, age-related condition, especially in people over 50, and is usually not sight-threatening on its own.
What Causes PVD?
PVD is most commonly caused by natural aging, but several factors can increase your risk:
- Age (especially over 50)
- Nearsightedness (myopia)
- Eye injuries or trauma
- Previous eye surgery (such as cataract surgery)
- Inflammation inside the eye
As the vitreous shrinks, it pulls away from the retina, sometimes causing noticeable visual symptoms.
Common Symptoms of PVD
PVD can happen suddenly, and its symptoms are often the first sign something has changed in your eye:
- Floaters (small shapes, dots, or cobweb-like shadows drifting across your vision)
- Flashes of light (especially in peripheral vision)
- Blurred or hazy vision
- A shadow or curtain effect (rare but serious)
While floaters and flashes are common in PVD, a sudden increase in these symptoms should never be ignored.
Is Posterior Vitreous Detachment Dangerous?
In most cases, PVD is benign and does not require treatment. However, complications can occur if the vitreous pulls too hard on the retina.
Potential complications include:
- Retinal tears
- Retinal detachment
- Vitreous hemorrhage
These conditions can threaten your vision and require urgent medical care.
When Should You See a Retina Specialist?
You should seek immediate evaluation if you experience:
- A sudden increase in floaters
- Frequent flashes of light
- A dark curtain or shadow in your vision
- Sudden vision loss
At Apex Retina Institute, our specialists use advanced imaging and diagnostic tools to quickly determine whether your symptoms are related to a simple PVD or something more serious.
How Is PVD Diagnosed?
Diagnosis typically involves a comprehensive dilated eye exam, allowing your retina specialist to examine the vitreous and retina in detail.
Additional imaging tests may include:
- Optical Coherence Tomography (OCT)
- Ultrasound imaging (if the view is obstructed)
Treatment Options for PVD
1. Observation (Most Common)
Most PVD cases require no treatment. Symptoms like floaters may gradually become less noticeable over time.
2. Monitoring for Complications
Your doctor may recommend follow-up visits to ensure no retinal tears or detachments develop.
3. Treatment for Complications
If complications arise, treatment may include:
- Laser therapy for retinal tears
- Cryotherapy (freezing treatment)
- Surgery for retinal detachment
Living with PVD
While PVD itself is usually harmless, adjusting to floaters can take time. Tips include:
- Moving your eyes up and down to shift floaters out of your central vision
- Maintaining regular eye exams
- Protecting your eyes from injury
- Staying alert to any sudden changes
Frequently Asked Questions (Q&A)
Q: Is PVD the same as retinal detachment?
A: No. PVD is the separation of the vitreous from the retina, while retinal detachment is when the retina itself pulls away from the back of the eye. However, PVD can sometimes lead to retinal detachment.
Q: Will floaters go away after PVD?
A: Floaters often become less noticeable over time as your brain adapts, but they may not disappear completely.
Q: Can PVD happen in both eyes?
A: Yes. If you experience PVD in one eye, it’s common for the other eye to develop it within a few years.
Q: Is PVD preventable?
A: PVD is a natural part of aging and generally cannot be prevented. However, routine eye exams can help detect issues early.
Q: How long do symptoms last?
A: Flashes may last a few weeks, while floaters can persist longer but usually become less bothersome over time.
Q: Should I be worried about flashes of light?
A: Occasional flashes can be normal with PVD, but new or frequent flashes should always be evaluated immediately.
Q: Does PVD require surgery?
A: No, not in most cases. Surgery is only needed if complications like retinal detachment occur.
Trust Your Vision to Specialists
If you’re experiencing symptoms of Posterior Vitreous Detachment or have concerns about your eye health, expert care is essential. Early detection can make all the difference in preserving your vision.
Contact Apex Retina Institute
Apex Retina Institute
2880 Atlantic Ave #290
Long Beach, CA 90806
📞 Phone: (562) 534-1777
🌐 Website: apexretinainstitute.com
👉 Request an Appointment:
https://apexretinainstitute.com/appointments/